Many commentators are increasingly concerned that the commitment to provide quality dental care to UK patients is becoming compromised.
Put simply the ethical principles under which UK dentists were trained and educated are increasingly difficult to achieve routinely in NHS, mixed and private practices.
As reported in the January 2016 by The Telegraph, a coalition of professionals from across the country argues that the NHS system is ‘unfit for purpose’ with millions of people seemingly going for long periods without even seeing a dentist, or ignorant of basic dental hygiene.
‘Far from improving, the situation has worsened to such an extent that charity groups normally associated with providing dental care in “third world” arenas now have to do so in England.’ – dentists’ letter to The Telegraph, 2016.
Whether UK dental clinicians are pressured by time and financial reward constraints to get their work completed, or whether there is less commitment within the General Dental Council (GDC) and its continuous professional development (CPD) requirements to continue the pursuit of clinical standards; there is a definite crisis looming in the reputation of UK dental services.
Clinical excellence should not be negotiable
Part one of this series of three articles will aim to review the current state of clinical care in the NHS, mixed and private practice arenas and the role that understanding communication systems plays in redirecting the profession to engage with their patients at a more empathetic level, thus creating trust and a higher acceptance of treatment recommendations, the very essence of private practice.
In the second article, we will present ways (both clinical and practice management related) to assist dental practices to move towards a more communicative, diagnostic based set of systems to spark a return to higher clinical standards and increased acceptance of ‘patient pays’ treatment recommendations.
Finally, in the third article, we will overview a way forward for the profession to start to return to clinical standards that we committed to on our graduation day; working with our teams and corporate owners to restore the quality of care and the quality of life that delivering quality dentistry provides.
Current state of play in the NHS
BBC News conducted a data analysis of more than 7,000 dental practices in England displaying information about new NHS patients; 48% were not accepting new adult patients, while 40% were not accepting new child patients.
The current NHS dental remuneration model is fundamentally incompatible with high clinical standards. Clinicians suffer stress from growing compliance issues; deterioration in perceived clinical freedoms and severe time constraints generated by ever more challenging UDA targets. This is leading to a crisis among NHS clinicians, whether they work for a corporate or an independently owned practice.
To escape from this clinical noose, the modern dentist needs to develop skills that will allow him or her to move their personal practice from a pure NHS model to a mixed model and then onto a full private model. The same argument applies to both the corporate environment and to independent practices.
The driving forces identified above will only get worse with the Governments’ known plans for the NHS dental service. The impact of those plans on the profession and the increased stress on individual dentists will lead to many more clinicians leaving the NHS, leaving the country or leaving dentistry altogether, and there may well be a future shortage of new EU and UK dentists to fill the vacancies left behind.
Types of practices in the UK
There are two types of general practice ownership in the UK, independent and corporate ownership; with three differing types of subgroups in these ownership models.
Available statistics would suggest that the share of over £7.1 billion (KPMG, 2017) gross dental revenue is spread over 43,000 plus registered dentists working in more than 12,000 practices.
• NHS: over 60% of practices grossing £3.5billion+ in NHS fees
• Mixed and private: around 40% grossing £3.6billion+ in private fees
• Corporates between them, receive over 24% of practice revenue.
Average per person dental spend is just over £90 in 2013/2014, which represents £44 paid by the NHS, £12 spent by patients on NHS dentistry, and £34 spent privately.
1: NHS practice
The Government contracts with the dentist to deliver a specific number of units of dental activity (UDAs) in a calendar year and pays in monthly instalments for the value of UDAs delivered. This traditional model remains the norm in over 60% of UK dental practices.
Whilst the system for delivering dental care in the NHS has been through many variations since its inception in 1948, it has never properly addressed the standards of care being delivered; simply fulfilling a contracted volume of UDAs in an NHS practice seen by many observers as a contributor to the reduction in the standards of care.
2: Mixed practice
The clinic delivers UDAs under an NHS GDS or PDS contract, but also delivers clinical work outside the
scope and financial constraints of UDAs via a non-NHS, independent, private practice model (fee per item or monthly payment plans).
The patient is generally advised at the chairside prior to treatment of the option to pay for higher standards of clinical care at an ‘out of pocket fee’ to the patient. The patient may be able to receive relief from some of these out of pocket expenses by using a payment plan such as Denplan.
This type of practice often involves the principal delivering largely private based care only and associates delivering the NHS treatment.
3: Private practice
The clinic only delivers private work with no NHS contract with the Government. Three levels of private practice exist.
a) Level one
This level one-type practice may accept emergency patients, pain management, single-tooth dentistry including extractions, fillings and root canals, depending on their business model (if in fact there is one). Scale and polish may be delivered by the dentist, rather than a hygienist or therapist as often seen in level two practices.
b) Level two A
The clinic engages with the patient in a semi-systematised way, including verbal treatment plans for the single tooth issues they present with. Treatment recommendations are communicated to the patient in a generic process usually downloaded from the practice management software systems in use.
The practice is more organised than the level one practices, often by the practice manager, and the staff have a better knowledge of the standards of care the practice wishes to deliver.
The team has more empathy in their patient care, better communication skills utilising photography (either intra-oral cameras or digital SLR systems) and a desire to include newer CAD/CAM technologies to address the recommendations of the diagnosis and treatment plans presented.
Hygienists are more evident in these level two A practices and the staff have expanded roles to support the clinicians, thereby optimising the clinician’s time availability.
c) Level two B
The practice engages more effectively with their patients through a highly-systematised delivery process and photographic communication systems are the foundations that enable patients to see their own mouths with clear evidence of issues and recommendations.
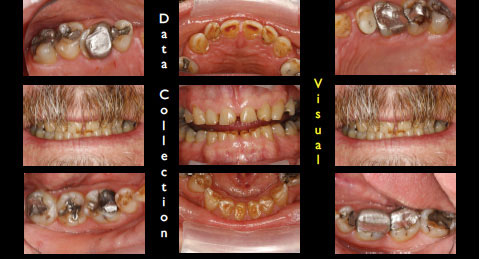
Photographic records are taken twice yearly with visual records updated after the completion of sequenced stages (Figure 2).
Full written treatment plans encompassing all diagnosed dental issues are provided with the sequencing of recommended care presented. This plan is then implemented and managed by the treatment coordinator.
Once the patient has completed part or all of their stages of treatment, they are placed in a ‘maintenance care and recall program’ under the guidance of the hygienist / therapist and overviewed by the clinician. At each recall the patient reviews with the clinical team their photographic records (which are updated at each stage of treatment completion) and any outstanding treatment is scheduled.
This practice can be totally systematised to deliver congruous, consistent care in a timely fashion by well-trained clinicians and teams with optimal profit levels.
d) Level three
This level of practice is mostly the home of the ‘restorative specialist’ practitioner. Some small numbers of high end general practices have also developed this type of clinic usually with outside consultants developing the internal patient management systems so that patients receive the most ideal and optimal care.
Corporate practice ownership
Modern corporate ownership interest in dental practices started some 20 years ago. Firstly, amongst a small number of clinicians with long-term views of the economies of scale purchasing practices would bring. Secondly, private equity groups started to purchase a number of practices based on a multiple of the clinic’s profit. As investors, they are attracted by the possibility of achieving scale economies through shared services, a shared talent pool and the option to vertically integrate into laboratories and other support services.
These corporates/consolidators provide back office support for the purchased clinics providing, payroll, accounts management and HR support. In return they create financial efficiencies within the clinics with better buying power of materials and lab work with an expected return on their investments of around 8-12% per annum.
Their collective body, The Association of Dental Groups (ADG) represents over 25 of these corporates / consolidators and their published objectives include:
• To ensure delivery of consistent quality outcomes for patients in a sustainable, high quality manner
• To support the Government’s aim to improve access to high quality dental care
• To adopt and maintain best practice across all their practices
• To work with the NHS to promote prevention of dental health problems
• To modernise working practices and maximise the roles of all dental professionals in dentistry
• To work with regulators and commissioners to ensure that regulation supports and responds to the changing needs.
Most corporate groups have created clinical boards and one of their roles is to improve the skill sets of clinicians.
The question we need to ask – is this really happening?
The role of communication in the modern practice
In 2012 the UK office of Fair Trading reported that dental patients often do not benefit from timely, clear and accurate information to make decisions regarding their choice of dentist or dental treatment – 82% of patients who recently received a course of dental treatment that incurred a charge did not receive a written treatment plan. – Office of NHS.
The more a dental practice engages with the move from NHS pay to a private practice user-pays, the more engaged with communication systems the clinical team needs to become as well as developing the ability to diagnose and present timely written treatment plans, which need to become the norm for the transitioning practice.
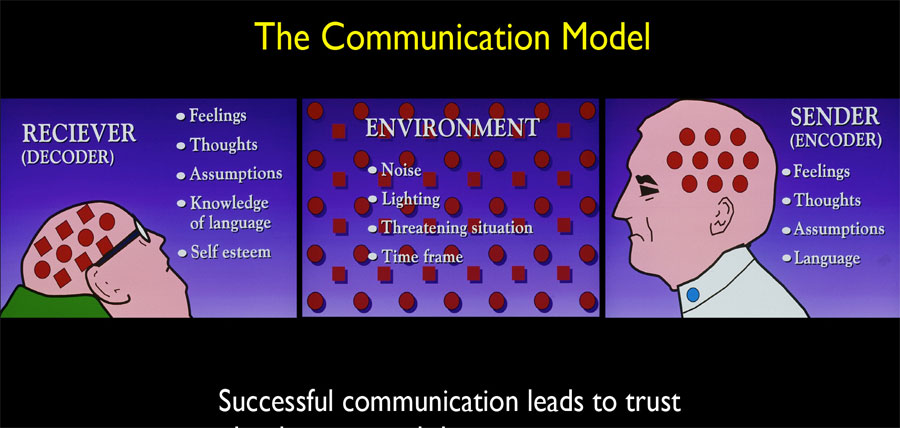
Figure 3 shows the traditional communication model in an NHS or type one private practice, showing the difficulties the environment creates in delivering clarity of explanation of simple and sometimes complex clinical situations.
The clinician is traditionally time poor and clearly influenced by their feelings and their thoughts at the time. Their ‘professional dental language’ is not clearly received by the generally nervous patient who does not speak this strange tongue and in the traditional challenging surgery environment, does not grasp clearly what the clinician is trying to tell them. Added to this communication nightmare are the differing personality styles of the clinician, the nursing team and the patients themselves.
The author has for many years taught ‘personality profiling’ (as named by Dr Tony Allesandra) and simplified it down to a basic set of four personality types defined by their emotive/openness levels (E) and their assertive/ directness levels (A).
When people act and react in social situations, they exhibit clues that help to define their behavioural styles. You can identify behavioural style by watching for the observable aspects of people’s behaviour – those verbal, vocal and visual actions that people display when others are present.
Identifying behavioural style is possible by classifying a person’s behavioural on two dimensions: openness and directness.
Openness (E) is the readiness and willingness with which a person outwardly shows emotions or feelings and develops interpersonal relationships.
Directness (A) refers to the amount of control and forcefulness that a person attempts to exercise over
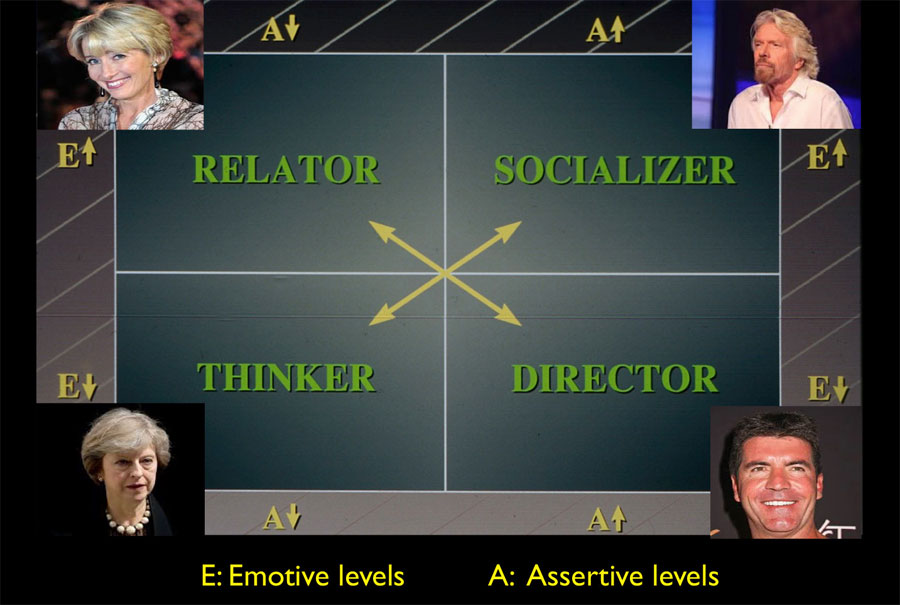
situations or other people, their thoughts and their emotions. – Dr Tony Allesandra, 1995
By understanding the personality profiles of the patient and the individuals in the clinical team, an opportunity to clearly communicate the way the patient is able to receive dental language is created.
Trust development is initiated and a higher acceptance of treatment recommendations becomes the norm when utilised with the photographic records presentation.
The whole team needs to be trained in this very important skill, most importantly the reception team who are taking calls from new patients and existing clients, either for recall exams or specific dental issues requiring care. This is the point at which the day’s schedule is set up and stress levels are either created or defused.
Evidence of shift to private
Private practice profits have crept ahead of NHS net profits for the first time in almost a decade. These figures come from the latest statistics released by NASDAL showing the average NHS practice makes a profit of £129,000 per principal compared with £131,000 for private practices.
Average gross fee income is up by £7,000 per NHS principal and £23,000 for private practice principals.
NASDAL has estimated that it costs £15,150 annually to meet Care Quality Commission (CQC) regulation requirements alone (this figure rises to £21,875 when registration fees and indemnity cover is added to this.). The need to cover the costs of CQC compliance is increasing at an exponential rate (the cost of compliance for dental practices committing to CQC recommendations has risen by 1,086% in the decade to 2016).
Clinicians need to look at increasing their net income through their private practice income to be able to afford these increasing costs, both to ensure patient safety and to maintain some semblance of lifestyle for themselves and their families.
With the trend showing a move towards the more private practices, it would serve both associates and principals to consider transitioning from an all-NHS to a mixed practice model, or from a mixed to all-private model to provide greater practice income.
Benefits of transition to mixed and full-private model
The benefits of transitioning from NHS to mixed and mixed to private practice include:
• Better diagnosis and increased time availability to discuss treatment options
• Ability to engage with the patient using communication skills (personality profiling) including photography techniques. This leads to better treatment planning and greater case acceptance
• Better quality of care delivery as a result of higher case acceptance levels combined with clinical training in newer technologies (such as the growing digital CAD/ CAM systems).
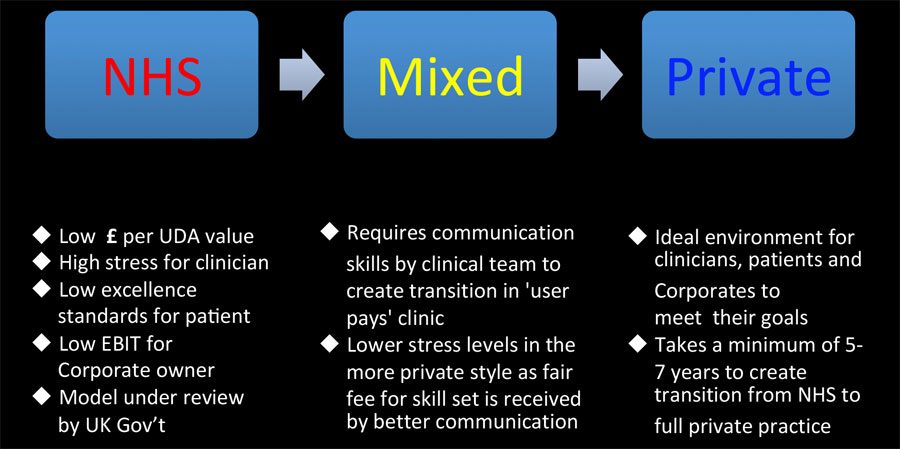
The positive and negatives of the three types of practice are summarised in Figure 6, indicating an increasing level of stress related to traditional NHS practices and an improvement in the dentist’s quality of life in the private practice model due to regaining control of their time available related to the delivery of care in a ‘user pays’ environment.
We start to see the private practice clinician regaining control of their time and stress management and hence the ability to spend this time in patient communication including treatment option discussions.
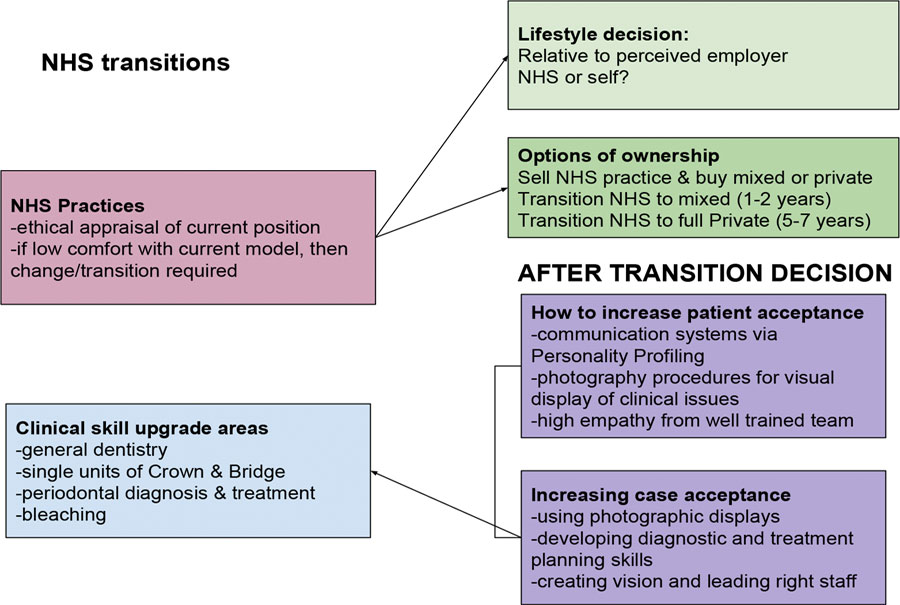
Transitioning in dental practices
The move from NHS to mixed and mixed to private practice is called the transition phase of practice growth.
The transition requires a commitment on behalf of the well-led team to change the way they communicate with patients as well as a change in the way data is captured at the initial and recall examination visit via photographic visual records.
As clinicians are generally not gifted with the ability to communicate clearly and concisely in a world of time constraints and fee constraints (NHS practice), they would benefit from simple photographic procedures to capture the patient’s dental state in a way they can see for themselves what clinicians are trying to communicate, ‘A picture tells a thousand words’.
Traditionally, students did not enter dental school on the basis of right brain skills. The entry process is based on the ability to pass A level exams creating an assessment of IQ (human intelligence) rather than the EI (emotional intelligence) skills of the right brain that enables us to communicate with our patients in a caring and sensitive manner. Photography offers a tool that can help bridge the communication gap.
to develop their treatment plans.
This change in emphasis towards the emotional aspects of human behaviour is relevant to dentistry as the context of dental care can be said to be inherently emotive. There are ‘unique stressors’, in care environments like dentistry, the consequence of the fact that work involves people, not objects, and in many cases dealing with vulnerable people – Broomfield et al, 1996.
By combining EI awareness, empathy and knowledge of personality profiling, the clinical team can communicate effectively and accelerate trust development. Only after this has been achieved can case acceptance occur. It is paramount that the foundations of sound diagnosis and ethical treatment planning underpin it. ‘Patients want to know how much we care before they care how much we know’
The transition process needs systems to be developed by the team, for the team and managed by the team. They then commit to this process so that the delivery of the patient care becomes systematised and consistent on at least an 80% eventuality basis.
This consistency of care combined with complete diagnosis and written treatment plans is what will lead to ‘word of mouth referrals’ and a greater acceptance of recommended treatment; hence the transition to a more ideal practice where the clinicians and their team are remunerated for their time and skills in a caring empathetic environment that rewards the team with better quality of life.
The ideal practice (Figure 8) receives its referrals from internal and external marketing activities, it has a consistent and reliable system to collect photographic records, X-ray records and periodontal records. It provides written recommendations via a treatment plan after thorough diagnostic evaluation and this is presented to the patient in a clearly communicated process, by a caring and empathetic dental team, using personality. Teams need to be trained and led with a clear vision (‘the why’ of the dental practice’s existence) presented to them clearly and the staff feel there is value in the change in direction of their practice, from a reactive mode of treatment (presenting treatment for the problem tooth) to a more inclusive mode of communicating with the patient

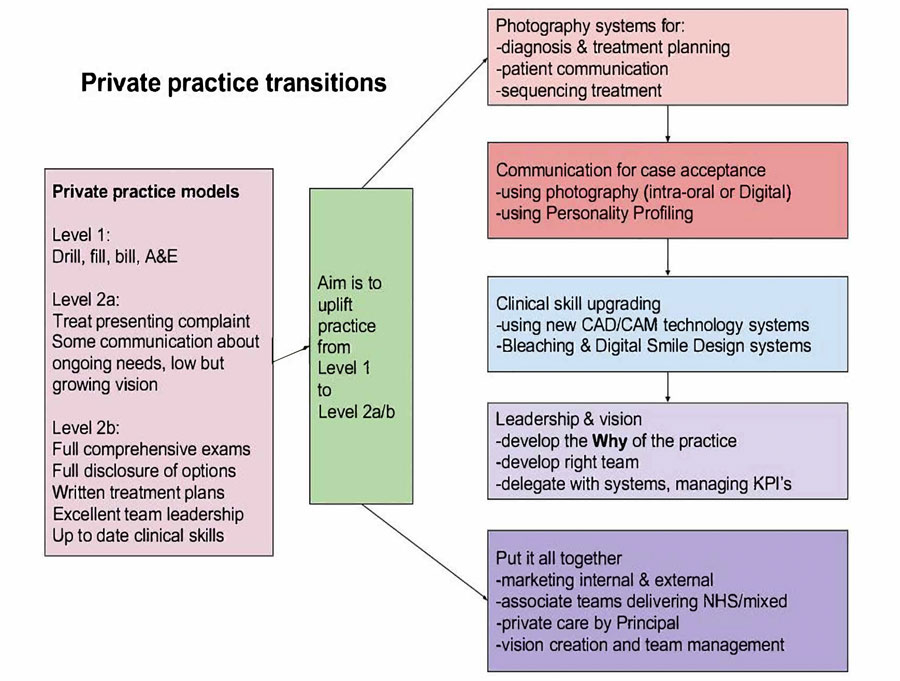
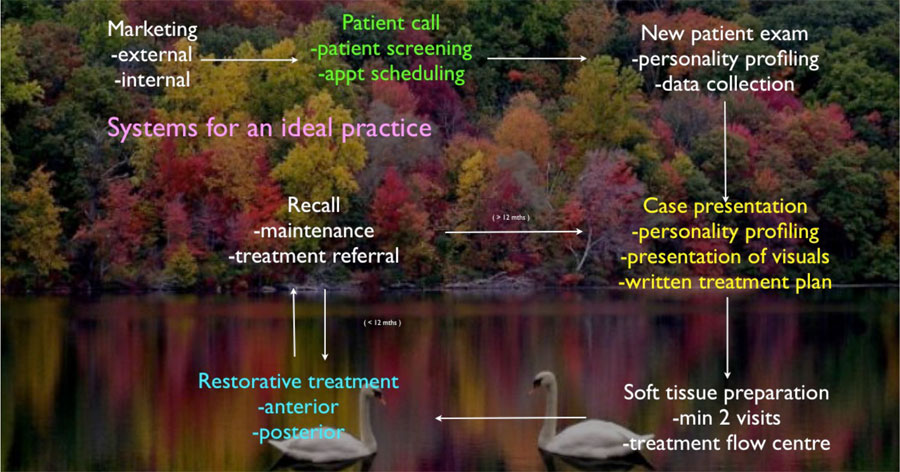
profiling communication skills under the vision set out by the senior clinician/practice owner/practice manager as defined by the practice’s ‘why’.
Conclusions
1: Many commentators claim that the commitment to provide quality dental care to UK patients is becoming compromised.
Factors contributing to this include:
• Less time availability and Government demands on dentists to deliver contracted UDAs, reduces ability to spend time delivering quality dentistry
• The stress of time demands and falling profits in dental practice due to increasing overheads are leading many dentists to consider early retirement due to stress and poor lifestyle
• There will be a shortage of dentists to fulfil the roles required to create profitable corporate and independently-owned practices.
2: Private practice dental profits have crept ahead of NHS net profits for the first time in almost a decade.
By developing internal systems with their dental teams, practices can communicate more successfully with their patients and hence increase the level of private practice ‘user-pays’ revenue through a transitioning process.
In article two we will outline the stages in the process of transitioning to a mixed/private approach that provides clinical teams with the skills to achieve this transition and secure the improved quality of life that is derived from a ‘team-orientated practice.’
You can create the practice you have always wanted.

Dr Derry Rogers
Dr Derry Rogers received his BDSc LDS from the University of Melbourne in 1977. He is the founder and past president of the Australian Society of Dental Aesthetics, a past accredited member of the American Academy of Cosmetic Dentistry, fellow of the International Academy of Facial Aesthetics and a member of the International Who’s Who of Professionals. He is the managing director of CD Marketing Products and the clinical director of The DR Institute, lecturing and consulting extensively around the world.

Dr john renshaw
Dr John Renshaw is a former chairman of the BDA, GDP for 47 years. He is cofounder of the Oral Care Consulting Group specialising in dental practice management, primary care dental service commissioning issues, legal compliance within the practice, complaints resolutions and the wider healthcare policy. He has been a major player in dental politics for over 30 years and was chairman of the British Dental Association from 2000 to 2006.